Understanding the burden of respiratory diseases in young children and comprehensive protection strategies from the earliest days of life
More than 70% of hospitalizations due to respiratory syncytial virus (RSV) occur within the first 6 months of life; pneumococcus accounts for approximately 50% of deaths from lower respiratory tract infections in children under 5 years old; globally, hundreds of millions of cases and over 2 million deaths related to respiratory diseases are recorded each year. These figures clearly indicate that young children are facing a “dual burden” from both viruses and bacteria from the earliest months of life, while their immune systems are still immature and a gap in early protection remains.
These important insights were shared by leading experts and physicians in Vietnam in the fields of pediatrics, infectious diseases, and vaccination at the scientific workshop “New Advances in the Prevention of Respiratory Diseases in Young Children,” held on April 23, 2026. The event provided a comprehensive perspective—from disease burden to modern, multi-layered preventive strategies beginning even before birth. It was organized by Tam Anh Research Institute in collaboration with Tam Anh General Hospital Group, with professional support from Pfizer Vietnam.
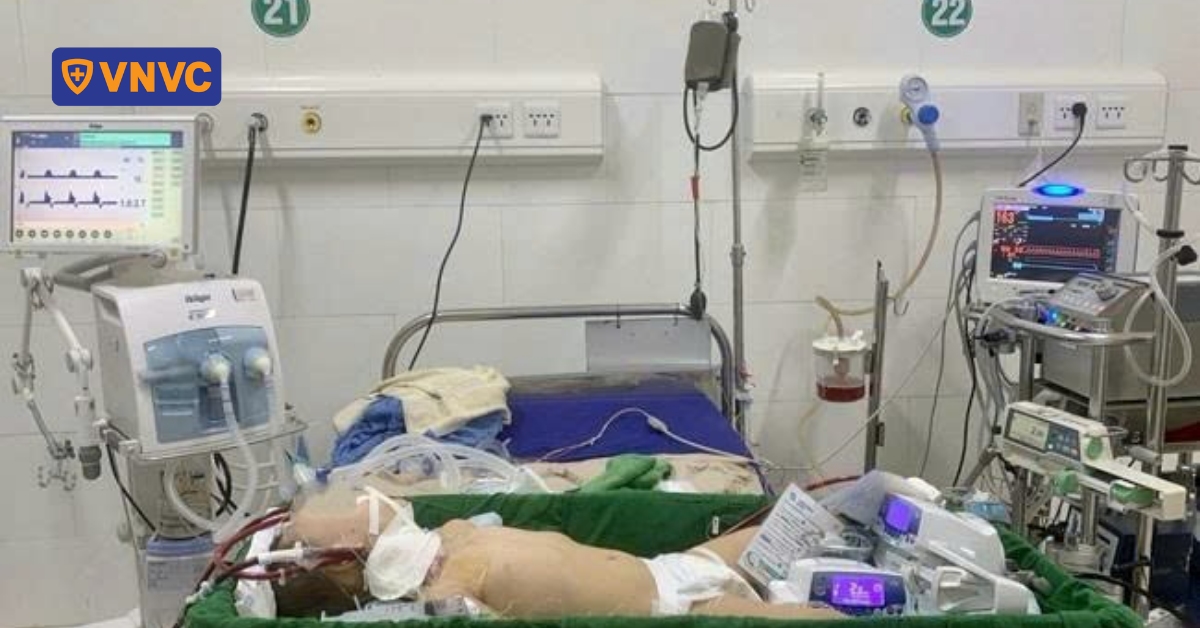
For decades, lower respiratory tract infections have remained one of the leading causes of severe illness, hospitalization, and death among young children worldwide. According to large-scale epidemiological analyses from the World Health Organization (WHO), the U.S. Centers for Disease Control and Prevention (CDC), and Global Burden of Disease (GBD) studies, hundreds of millions of lower respiratory tract infections are recorded globally each year, with over 2 million deaths, the majority occurring in children under 5 years old.
Among these, pneumococcus is estimated to account for about half of all deaths due to lower respiratory tract infections in children under 5. Data from the 2021 Global Burden of Disease study show that despite significant progress in disease control, the world still records approximately 433 million lower respiratory tract infections and 2.18 million deaths annually.
Meanwhile, RSV is identified as the leading viral cause of pneumonia in children under 5 years old, particularly in low- and middle-income countries, accounting for up to 98% of pneumonia-related deaths in children according to UNICEF, and associated with around 70% of hospitalizations in infants under 6 months of age. Statistics indicate that RSV accounts for approximately 31.2% of viral pneumonia cases, far exceeding other pathogens such as Rhinovirus, hMPV, Parainfluenza, or Influenza.
In middle-income countries such as Vietnam, this burden becomes even more pronounced, as environmental conditions, population density, unequal access to healthcare services, and uneven vaccination coverage continue to facilitate sustained circulation of pathogens. In this context, medical experts emphasize: “It is time for a more comprehensive, earlier, and more precise approach to preventing respiratory diseases in young children.”
Respiratory viruses and bacteria “coexist” with children from the earliest months of life
Opening the workshop, Dr. Truong Huu Khanh, Vice President of the Ho Chi Minh City Infectious Diseases Society, raised a fundamental but often overlooked issue: young children do not face individual pathogens in isolation, but rather a complex microbial ecosystem in which viruses and bacteria coexist, interact, and amplify disease risk.
From birth, children are exposed to a wide range of microorganisms in their environment, from viruses such as RSV and Rhinovirus to bacteria such as pneumococcus (Streptococcus pneumoniae), Haemophilus influenzae, and Staphylococcus aureus. Notably, the immune system of newborns is still immature, both in innate and adaptive immunity, limiting their ability to control pathogens effectively.
Within this broader picture, RSV and pneumococcus emerge as the two “central drivers” of the respiratory disease burden in young children. International studies show that RSV is the leading cause of lower respiratory tract infections in infants, particularly bronchiolitis and viral pneumonia. Hospitalization rates due to RSV peak in infants aged 1–2 months, with more than 70% of cases occurring within the first 6 months of life, when vaccine-derived protection is still largely absent.
Beyond its high incidence, RSV is also one of the leading causes of death in children under 1 year old, second only to certain major infectious diseases such as malaria in some regions. Notably, over 97% of RSV-related deaths occur in low- and middle-income countries, clearly reflecting disparities in access to preventive and treatment measures.
Alongside RSV, pneumococcus continues to be the leading cause of pneumonia-related deaths in young children. GBD data indicate that pneumococcus accounts for approximately half of all deaths due to lower respiratory tract infections in children under 5.
Importantly, these two pathogens do not act independently. A growing body of scientific evidence shows that viral infections (especially RSV) can facilitate bacterial invasion and lead to more severe disease. Viral–bacterial co-infection or sequential infection increases the risk of complications, prolongs hospitalization, and raises treatment costs.
In Nha Trang, studies show that children with pneumonia co-infected with viruses such as RSV or influenza have pneumococcal loads 15 times higher than those without co-infection. In Thai Binh, 87% of children under 5 with community-acquired pneumonia were infected with multiple pathogens simultaneously, including RSV (24%) and pneumococcus (45%). Data from Children’s Hospital 1 also indicate that more than 80% of children with RSV infection had concurrent bacterial infections, significantly increasing the likelihood of requiring intensive care.
Therefore, focusing on a single pathogen is insufficient to reduce disease burden. Instead, a multi-pathogen prevention strategy is required, capable of covering both viruses and bacteria from the earliest stages.

RSV and pneumococcus are two dangerous respiratory pathogens in young children, capable of rapid progression and severe complications, threatening health and life if not prevented in a timely manner.
The “window of vulnerability” and a turning point with prenatal protection strategies
One of the key concepts highlighted in the presentation by MSc., MD Nguyen Canh Chuong, Director of the Training and Referral Center at Hanoi Obstetrics Hospital, is the “window of vulnerability.” This refers to the period from birth through the first months of life, when the immune system is not yet fully developed and has not responded to the basic vaccination schedule.
This is the period when children are at the highest risk of severe respiratory infections, particularly RSV. Meanwhile, many important vaccines are only administered starting from 2 months of age (as early as 6 weeks), creating a significant immunity gap.
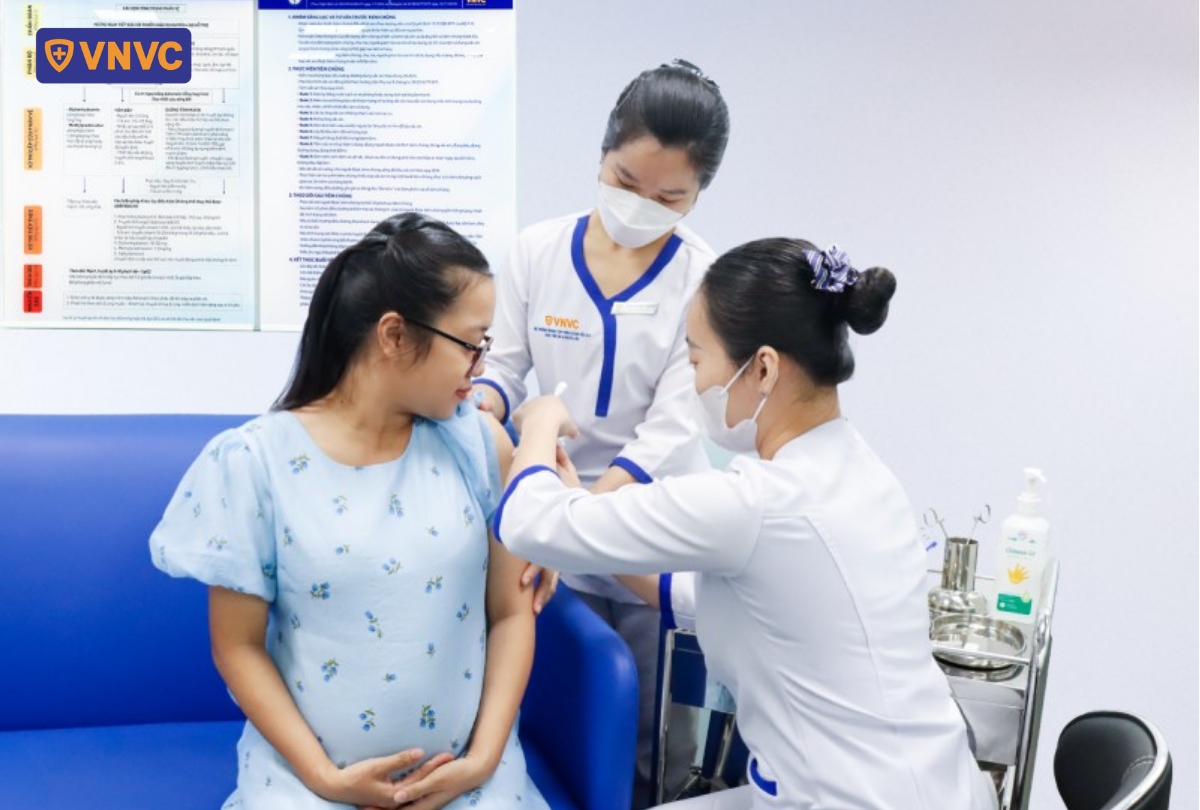
To address this gap, modern medicine has shifted toward a foundational strategy: protecting children in utero through maternal vaccination. This strategy is based on natural immunological physiology: maternal IgG antibodies can cross the placenta to the fetus, providing passive immunity at birth. After delivery, IgA antibodies in breast milk continue to protect the respiratory and gastrointestinal mucosa.
Leading health organizations such as WHO, CDC, and the American College of Obstetricians and Gynecologists recommend vaccination during pregnancy as a dual-protection measure—for both mother and newborn. Among these, RSV vaccination for pregnant women is considered a breakthrough. Phase 3 clinical trials and real-world data have demonstrated significant protective efficacy, reducing the risk of RSV-related lower respiratory tract infection hospitalization by more than 70% in infants during the first 6 months of life.
In Australia and Argentina, RSV vaccines have been included in national immunization programs and are provided free of charge to eligible pregnant women. Implementation has shown clear effectiveness. In Australia, RSV cases in young children decreased by nearly 40%, from 45,838 cases (February–May 2024) to 27,921 cases during the same period the following year. In Argentina, lower respiratory tract infections from all causes decreased by 41% compared to the same period of the previous year. In the United States, estimates suggest that with 100% maternal vaccination coverage, RSV vaccination could prevent approximately 24,520 hospitalizations and 47 deaths annually in children under 1 year old.
In addition to efficacy, safety data show no significant increase in serious adverse events in either mothers or newborns, reinforcing confidence in the feasibility of this strategy in clinical practice.
Other preventive solutions, such as monoclonal antibodies (e.g., Nirsevimab or Palivizumab), also contribute to enhanced protection, particularly for high-risk or premature infants.
These advances reflect a clear shift: from “treating disease after it occurs” to “proactively preventing disease before birth.”
The role of next-generation pneumococcal vaccines in a multi-layered strategy
If RSV represents viral pathogens, pneumococcus is the “cornerstone” among bacterial respiratory pathogens. According to PhD, MD Nguyen An Nghia, Deputy Head of the Infectious–Neurology Department at Children’s Hospital 1, Ho Chi Minh City, controlling pneumococcus plays a critical role in reducing the burden of pneumonia and severe complications in young children.
Over the past decade, pneumococcal conjugate vaccines (PCVs) have demonstrated outstanding global effectiveness, significantly reducing invasive pneumococcal diseases such as meningitis, sepsis, and severe pneumonia. Many countries have reported reductions ranging from 57% to nearly 100% in cases caused by vaccine-covered serotypes.
However, changes in serotype distribution over time necessitate the development of next-generation vaccines with broader coverage. The 20-valent pneumococcal conjugate vaccine (PCV20) represents such an advancement, covering over 66.5% of disease-causing serotypes in children under 5 globally—substantially higher than PCV10 (10.7%), PCV13 (37.4%), or PCV15 (44.5%), and even reaching 87.2–94% in some studies in Vietnam between 2019 and 2022.
“Pneumococcal conjugate vaccines also help reduce the overall burden of respiratory diseases,” emphasized Dr. Nguyen An Nghia, citing studies showing that pneumococcal vaccination reduces all-cause pneumonia by 47% and RSV-related cases by 29% in children under 5. This highlights the close relationship between viral and bacterial pathogens in respiratory diseases and confirms the synergistic effectiveness of vaccination strategies.
Importantly, pneumococcal vaccines do not replace RSV prevention measures but significantly reduce the overall burden of respiratory diseases, including virus-associated pneumonia. Therefore, the optimal strategy is not to choose between interventions, but to combine them in a rational and evidence-based manner.
Toward a comprehensive prevention model: from isolated to integrated approaches
In concluding the workshop, Chairperson Dr. Bach Thi Chinh, Medical Director of the VNVC Vaccination System, emphasized a guiding message: “Prevention of respiratory diseases in young children should be approached as a continuous system, beginning before birth and extending throughout the early years of life.”
Accordingly, an effective prevention strategy should include:
- Early protection during pregnancy through maternal vaccination;
- Full and timely vaccination for children, particularly pneumococcal vaccines;
- Application of modern preventive solutions such as monoclonal antibodies for high-risk groups;
- Strengthening communication and health education to improve community awareness and proactive prevention.
The core message emphasized is that no single solution is sufficient to control the entire burden of respiratory diseases in young children. Only through a multi-layered, multi-pathogen approach grounded in solid scientific evidence can the risks of severe illness, hospitalization, and death be minimized. Pregnant women and newborns are also advised to seek consultation at reputable healthcare facilities such as Tam Anh General Hospital or the VNVC Vaccination System for appropriate assessment and vaccination recommendations, ensuring optimal safety and effectiveness in respiratory disease prevention.













